What are Kidney Stones?

Kidney stones form when the urine becomes too concentrated causing crystals to form and aggregate into stones. Stones can vary in size and those >4mm are unlikely to pass on their own.
Are there different types of Kidney Stones?
There are three main types of stones:
- Calcium stones formed from calcium combined with oxalate or phosphate are the most common type of kidney stone.
- Struvite stones, which are caused by a urine infection. These are often staghorn-shaped and can be quite large.
- Uric acid stones are found more often in men than women. Patients with gout, or high blood uric acid, diabetes, and patients undergoing chemotherapy are at higher risk of these types of stones, although they can form in people with none of these conditions.
Occasionally stones are due to rare hereditary metabolic conditions e.g. cystine stones or may be related to medication.
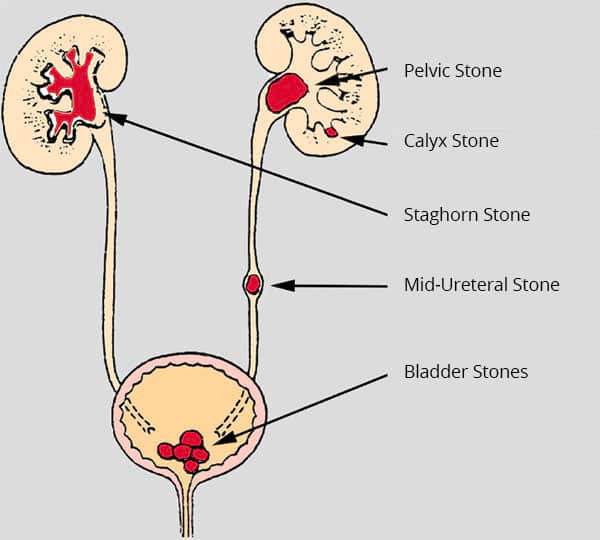
What causes Kidney Stones?
In most cases there is no known reason why a stone is formed.
A kidney stone can form when substances such as calcium, oxalate, cystine or uric acid are at high levels in the urine. However, stones can also form if these chemicals are at normal levels.
Medications used for treating some medical conditions such as kidney disease, cancer or HIV can also increase your risk of developing kidney stones.
A small number of people get kidney stones because of a medical condition. These conditions can lead amounts of calcium, oxalate, cystine or uric acid that are at high levels in the body.
Who is affected by Kidney Stones?
Kidney stones are one of the most common disorders of the urinary tract. About 4-8% of Australians suffer from kidney stones at some time. The lifetime risk of developing kidney stones is 1 in 10 for Australian men and 1 in 35 for women. The chance of developing a stone increases if you have a family history of stones and as you age. Urinary tract stones are more common in children in developing countries and amongst indigenous Australians.
After having one kidney stone, the chance of getting a second stone is about 5-10% each year. About 30-50% of people with a first kidney stone will get a second one within five years and then the risk declines. However, some people keep getting stones their whole lives.
What problems do Kidney Stones cause?
Kidney stones may not cause any symptoms but when they cause a blockage, infection or inflammation symptoms and complications can occur. When a kidney stone causes a blockage in the flow of urine, severe pain can occur (renal colic). A severe blockage especially if there is an underlying infection can damage and sometimes cause failure of the blocked kidney. Stones increase the chance of urinary and kidney infection and can result in the serious condition of septicaemia, if germs spread into the blood stream.
What are the symptoms of Kidney Stones?
Not all kidney stones cause discomfort but pain is usually the first sign. It usually begins when a stone moves from where it has formed into the urinary tract. This pain, known as ‘renal colic’, is a gripping pain in the back just below the ribs. It can spread around to the front of the body and sometimes towards the groin.
Other symptoms include:
- Blood in the urine, which can be seen by the eye or found when tested.
- Nausea and vomiting.
- Shivers, sweating and fever, cloudy or bad smelling urine if there is an accompanying infection.
- ‘Gravel’ in the urine, which is made of small uric acid stones.
- An urgent feeling of needing to urinate.
How are Kidney Stones detected?
Many stones are found by chance during tests for other conditions. Kidney stone tests may include:
- Ultrasound.
- CT scans.
- X rays including an intravenous pyelogram or IVP, where dye is injected into the bloodstream before the x-rays are taken.
Analysis of a stone is very useful, so if you do pass a stone, try to collect a sample and take it to your doctor. Detecting and diagnosing stones helps to decide on the treatment. Urine and blood tests can assist in finding out the cause of the stone.
How are Kidney Stones treated?
The type of treatment needed for a kidney or ureteric stone will depend on a number of factors that must be assessed by a urologist. These include the site of the stone (where it is), the size of the stone(s), the type of stone, how long it has been present, your symptoms, any associated infection, and your medical history.
Most kidney stones will be small enough (no more than 4mm) to be passed out in your urine. It may be possible to treat these at home. However, small kidney stones may still cause pain. The pain from smaller kidney stones usually lasts a couple of days and disappears when the stone has been passed.
Medication
If you have severe pain, your GP may inject you with a painkiller. A second dose can be given after half an hour if you are still experiencing pain
Medication can also be injected to treat the symptoms of nausea (feeling sick) and vomiting. This is called an anti-emetic (anti-sickness) medication.
You may also be given a prescription for painkillers, anti-emetics, or both, to take at home.
Self-Care
If you are sent home to wait for your kidney stone to pass, you may be advised to try to collect the stone from your urine.
You can do this by filtering your urine through gauze or a stocking. The stone can be given to your GP to help them determine any further treatment you may need. You should drink enough water to make your urine colourless. If your urine is yellow or brown, you are not drinking enough.
Admission to Hospital
If your kidney stone has moved into your ureter and it is causing severe pain, your GP or Urologist may admit you to hospital for treatment.
This may be necessary if:
- You are at an increased risk of your kidneys failing (for example, because you only have one kidney).
- Your symptoms do not improve within an hour of being given painkillers or anti-sickness medication.
- You are dehydrated and you are vomiting too much to keep fluids down.
- You are pregnant.
- You are over 60 years of age.
Treating large Kidney Stones
If a kidney stone is too big to be passed naturally (6-7mm in diameter or larger), you may need to have treatment to remove it another way.
This could include:
- Extracorporeal shock wave lithotripsy (ESWL).
- Ureterorenoscopy.
- Percutaneous nephrolithotomy (PCNL).
- Open surgery.
These procedures are explained in more detail below. The type of treatment you have will depend on the size and location of your stones.
Extracorporeal Shock Wave Lithotripsy (ESWL)
Extracorporeal Shock Wave Lithotripsy (ESWL) is the most common way of treating kidney stones that cannot be passed in the urine.
It involves using X-rays (high-energy radiation) or ultrasound (high-frequency sound waves) to pinpoint where a kidney stone is. A machine then sends shock waves of energy to the stone to break it into smaller pieces so it can be passed in your urine.
ESWL can be an uncomfortable form of treatment, so it is usually performed after giving painkilling medication or under a general anaesthetic.
You may need more than one session of ESWL to treat your kidney stones successfully. ESWL is up to 60-80% effective for stones that are up to 20mm (= in diameter.
Ureterorenoscopy
If a kidney stone is stuck in your ureter (tube that carries waste products from your kidneys to your bladder), you may need to have Ureterorenoscopy.
Ureterorenoscopy is also sometimes known as retrograde intrarenal surgery (RIRS).
It involves passing a long, thin telescope called a ureteroscope through your urethra (the tube urine passes through out of the body) and into your bladder. It is then passed up into your ureter to where the stone is stuck.
The surgeon may either try to gently remove the stone using another instrument, or they may use laser energy to break the stone up into small pieces so that it can be passed naturally in your urine.
Ureterorenoscopy is performed under general anaesthetic, so you should not drive or operate machinery for up to 48 hours after the procedure.
For stones up to 15mm (0.6in), ureterorenoscopy is effective in 80% of cases. You may need a plastic tube called a stent to be inserted inside you temporarily to allow the stone fragments to drain into the bladder.
Percutaneous Nephrolithotomy (PCNL)
Percutaneous Nephrolithotomy (PCNL) is an alternative procedure that may be used for larger stones. It may also be used if ESWL is not suitable (for example, because the person being treated is obese).
PCNL involves using a thin telescopic instrument called a nephroscope. An incision (cut) is made in your back. The nephroscope is passed through the incision and into your kidney. The stone is either pulled out or broken into smaller pieces using a laser or pneumatic energy.
It is always performed under general anaesthetic (you are put to sleep), which means that you should not drive or operate machinery for up to 48 hours after the procedure.
PCNL is 86% effective for stones that are 21-30mm (0.8-1.2in) in diameter.
OPEN SURGERY
Nowadays, it is rare for people to have open surgery for kidney stones (less than 1% of cases require this type of surgery). It is usually used if there is a very large stone or abnormal anatomy.
It involves making an incision in your back to gain access to both your ureter and your kidney. The kidney stone can then be removed.
Treating Uric Acid Stones
If you have a uric acid stone, you may be advised to drink around three litres of water each day to try to dissolve it.
Uric acid stones are much softer than other types of kidney stone, and they can be made smaller if they are exposed to alkaline fluids.
You may need to take some medication to make your urine more alkaline before the uric acid stone starts to dissolve.
How can I prevent Kidney Stones?
If you have had one stone already, these are some tips for reducing your risk of further stones:
- Talk to your doctor about the cause of previous stones.
- Ask your doctor to check what medications you are on to see if they might be causing your stones. Do not stop your medications without talking to your doctor.
- Get quick and proper treatment of urinary infections.
- Avoid dehydration. Drink enough fluids to keep your urine volume at or above two litres a day. This can halve your risk of getting a second stone by lowering stone-forming chemicals.
- Avoid too much tea or coffee.
- Citrus juices may reduce the risk of some stones, particularly orange, grapefruit and cranberry.
- Mineral water cannot cause kidney stones because it contains only trace elements of minerals.
- Reducing salt often lowers the risk of calcium containing stones. Don’t add salt while cooking and leave the saltshaker off the table. Choose low or no salt processed foods.
- Lowering calcium below that of a normal diet is only necessary in some cases where absorption of calcium from the bowel is high. A low calcium diet has not been shown to be useful in preventing the recurrence of kidney stones and may worsen the problem of weak bones. People with calcium containing stones may be at greater risk of developing weak bones and osteoporosis. Discuss this risk with your doctor.
- Don’t drink more than 1 litre per week of drinks with phosphoric acid, which is used to flavour carbonated drinks such as cola and beer.
Always talk to you doctor before making changes to your diet.